What Is An ACL Tear?
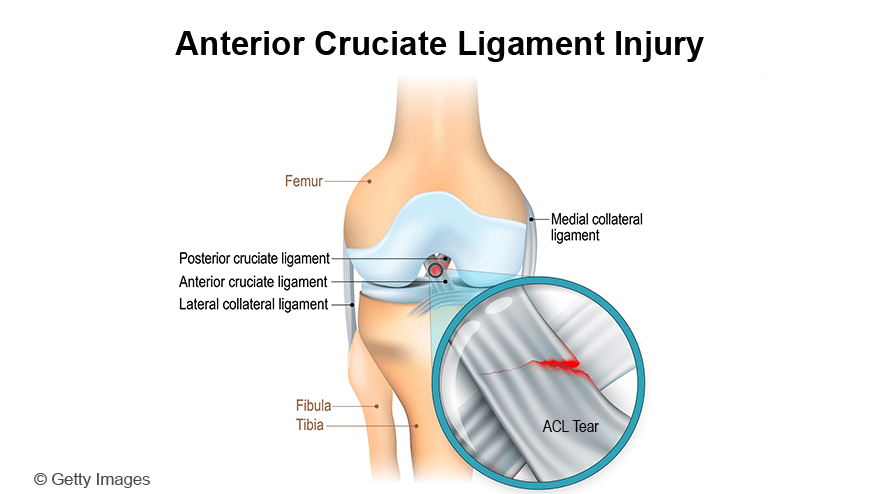
The ACL is one of the major bands of tissue (ligaments) connecting the thigh bone (femur) to the shin bone (tibia) at the knee joint. It can tear if you:
How Does It Feel?
When you tear the ACL, you may feel a sharp, intense pain or hear a loud “pop” or snap. You might not be able to walk on the injured leg because you can’t support your weight through your knee joint. Usually, the knee will swell immediately (within minutes to a few hours), and you might feel that your knee “gives way” when you walk or put weight on it.
How Is It Diagnosed?
Immediately following an injury, you may be examined by a physical therapist, athletic trainer, or orthopedic surgeon. If you see your physical therapist first, your therapist will conduct a thorough evaluation that includes reviewing your health history. Your physical therapist will ask:
Your physical therapist may perform gentle “hands-on” tests to determine the likelihood that you have an ACL tear, and may use additional tests to assess possible damage to other parts of your knee.
An orthopedic surgeon may order further tests, including magnetic resonance imaging (MRI), to confirm the diagnosis and rule out other possible damage to the knee.
Surgery
Most people who sustain an ACL tear will undergo surgery to repair the tear; however, some people may avoid surgery by modifying their physical activity to relieve stress on the knee. A select group can actually return to vigorous physical activity following rehabilitation without having surgery.
Your physical therapist, together with your surgeon, can help you determine if nonoperative treatment (rehabilitation without surgery) is a reasonable option for you. If you elect to have surgery, your physical therapist will help you prepare both for surgery and to recover your strength and movement following surgery.
How Can a Physical Therapist Help?
Once an ACL tear has been diagnosed, you will work with your surgeon and physical therapist to decide if you should have surgery, or if you can recover without surgery. If you don’t have surgery, your physical therapist will work with you to restore your muscle strength, agility, and balance, so you can return to your regular activities. Your physical therapist may teach you ways to modify your physical activity in order to put less stress on your knee. If you decide to have surgery your physical therapist can help you before and after the procedure.
Treatment Without Surgery
Current research has identified a specific group of patients (called “copers”) who have the potential for healing without surgery following an ACL tear. These patients have injured only the ACL, and have experienced no episodes of the knee “giving out” following the initial injury. If you fall into this category, based on the specific tests your physical therapist will conduct, your therapist will design an individualized physical therapy treatment program for you. It may include treatments such as gentle electrical stimulation applied to the quadriceps muscle, muscle strengthening, and balance training.
Treatment Before Surgery
If your orthopedic surgeon determines that surgery is necessary, your physical therapist can work with you before and after your surgery. Some surgeons refer their patients to a physical therapist for a short course of rehabilitation before surgery. Your physical therapist will help you decrease your swelling, increase the range of movement of your knee, and strengthen your thigh muscles (quadriceps).
Treatment After Surgery
Your orthopedic surgeon will provide postsurgery instructions to your physical therapist, who will design an individualized treatment program based on your specific needs and goals. Your treatment program may include:
Bearing weight – Following surgery, you will use crutches to walk. The amount of weight you are allowed to put on your leg and how long you use the crutches will depend on the type of reconstructive surgery you have received. Your physical therapist will design a treatment program to meet your needs and gently guide you toward full weight bearing.
Icing and compression – Immediately following surgery, your physical therapist will control your swelling with a cold application, such as an ice sleeve, that fits around your knee and compresses it.
Bracing – Some surgeons will give you a brace to limit your knee movement (range of motion) following surgery. Your physical therapist will fit you with the brace and teach you how to use it safely. Some athletes will be fitted for braces as they recover and begin to return to their sports activities.
Movement exercises – During your first week following surgery, your physical therapist will help you begin to regain motion in the knee area, and teach you gentle exercises you can do at home. The focus will be on regaining full movement of your knee. The early exercises help with increasing blood flow, which also helps reduce swelling.
Electrical stimulation – Your physical therapist may use electrical stimulation to help restore your thigh muscle strength, and help you achieve those last few degrees of knee motion.
Strengthening exercises – In the first 4 weeks after surgery, your physical therapist will help you increase your ability to put weight on your knee, using a combination of weight-bearing and non-weight-bearing exercises. The exercises will focus on your thigh muscles (quadriceps and hamstrings) and might be limited to a specific range of motion to protect the new ACL. During subsequent weeks, your physical therapist may increase the intensity of your exercises and add balance exercises to your program.
Balance exercises – Your physical therapist will guide you through exercises on varied surfaces to help restore your balance. Initially, the exercises will help you gently shift your weight on to the surgery leg. These activities will progress to standing on the surgery leg, while on firm and unsteady surfaces to challenge your balance.
Return to sport or activities – As athletes regain strength and balance, they may begin running, jumping, hopping, and other exercises specific to their individual sport. This phase varies greatly from person-to-person. Physical therapists design return-to-sport treatment programs to fit individual needs and goals.
Can This Injury or Condition Be Prevented?
Much of the research on ACL tears has been conducted with female collegiate athletes, because women are 4 to 6 times more likely to experience the injury. Preventive physical therapy programs have proven to lower ACL injury rates by 41% for female soccer players. Researchers have made the following recommendations for a preventive exercise program:
Although most exercise studies have been conducted with female athletes, the findings may benefit male athletes as well.




